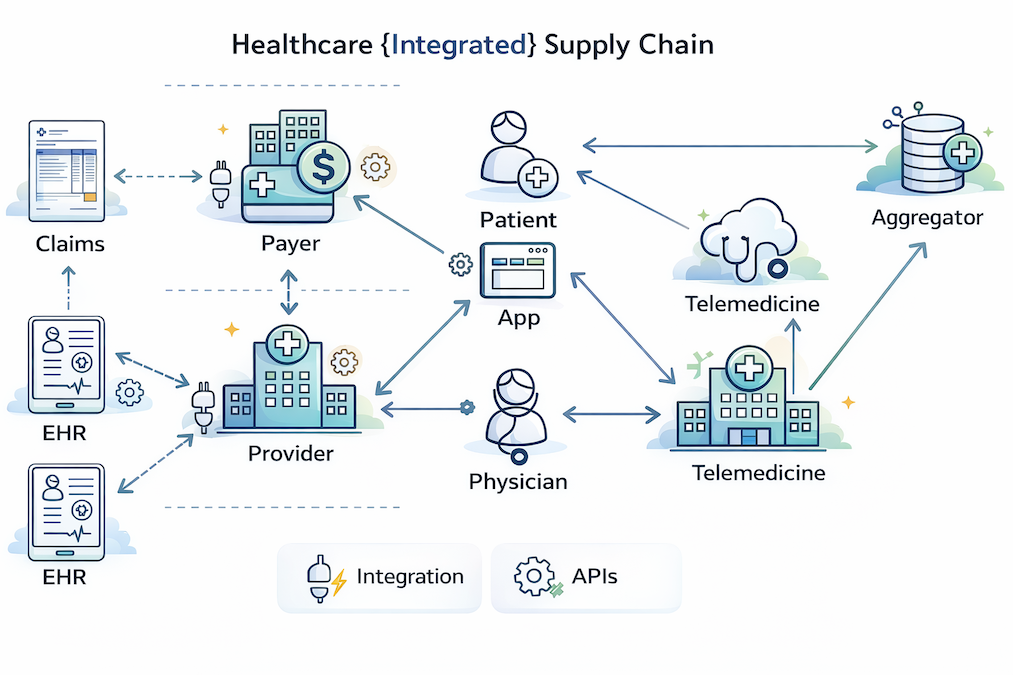
The healthcare industry is entering a new regulatory era—one that prioritizes data accessibility, interoperability, and patient control. As new federal mandates continue to evolve into 2026 and 2027, hospitals, clinics, and provider networks face increasing pressure to modernize their Electronic Health Record (EHR) systems.
At the center of these changes is FHIR (Fast Healthcare Interoperability Resources)—a standard that is rapidly becoming the foundation for compliance and future-ready healthcare infrastructure.
For organizations still relying on legacy EMR/EHR systems, the message is clear:
Modernization is no longer optional—it is required.
Recent and upcoming regulatory frameworks are reshaping how healthcare data must be managed and shared. These include:
The Regulatory Shift: What’s Changing in 2026–2027?
- CMS interoperability mandates
- Patient Access API requirements
- Prior Authorization automation rules
- Data-sharing requirements between providers and payers
- Information blocking enforcement
These regulations are designed to ensure:
- Patients have real-time access to their health data
- Providers can exchange data seamlessly
- Administrative processes are digitized and automated
FHIR is the standard that enables all of this.
What Makes FHIR-Based EHR Systems Different?
Traditional EHR systems were built as closed ecosystems, making data sharing complex, slow, and expensive.
FHIR-based systems are fundamentally different. They are built around:
- Open APIs for data exchange
- Standardized data formats (FHIR resources)
- Real-time interoperability
- Cloud-ready architectures
This makes them inherently aligned with modern regulatory requirements.
How a FHIR-Based EHR Architecture Works
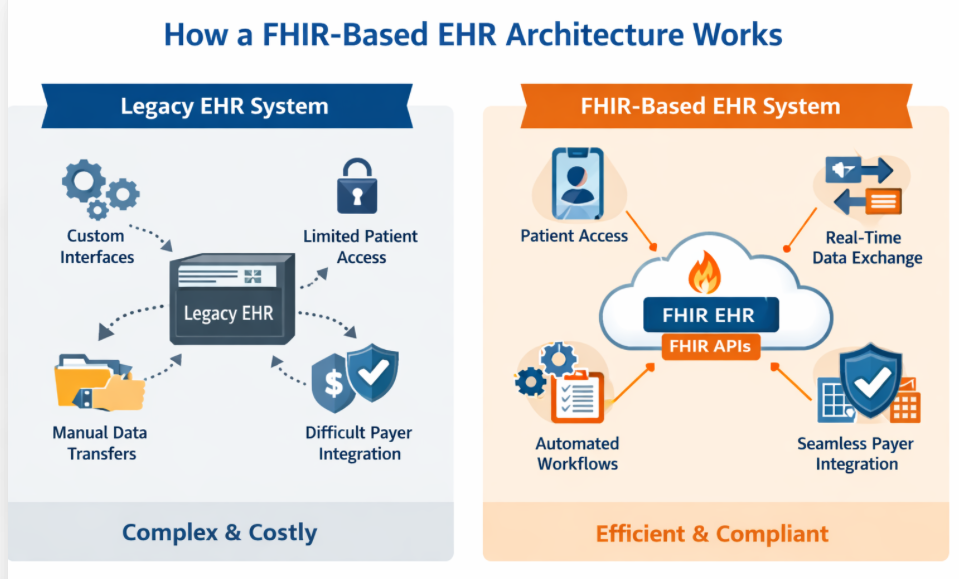
In a FHIR-enabled environment:
- The EHR acts as a central data source
- Data is exposed through secure FHIR APIs
- External systems (apps, payers, providers) can access data in real time
- Patients can retrieve their health data through approved applications
This architecture ensures compliance while enabling flexibility and innovation.
Why Legacy EHR Systems Will Struggle to Keep Up
Many existing EHR systems were not designed with interoperability in mind. As a result, they face significant challenges:
- High cost of retrofitting APIs
- Limited ability to meet real-time data requirements
- Complex integration with payer systems
- Increased risk of non-compliance
Organizations attempting to “patch” legacy systems often find themselves facing:
- Escalating IT costs
- Delayed compliance timelines
- Operational inefficiencies
At a certain point, upgrading becomes more expensive than transitioning to a modern FHIR-based platform.
Key Compliance Benefits of FHIR-Based EHR Systems
1. Built-In Patient Access APIs
Regulations require patients to have easy, digital access to their health records.
FHIR-based systems enable:
- Mobile app integration
- Real-time data access
- Secure patient authorization
This eliminates the need for costly custom patient portals.
2. Automated Prior Authorization Workflows
New CMS rules emphasize automation in prior authorization.
FHIR enables:
- Real-time data exchange with payers
- Faster approvals
- Reduced administrative burden
This directly improves both compliance and operational efficiency.
3. Reduced Risk of Information Blocking Violations
Information blocking regulations require providers to share data when requested.
FHIR-based systems ensure:
- Standardized data access
- Secure and compliant sharing
- Transparent data exchange processes
This significantly reduces legal and financial risk.
4. Easier Integration with Payers and Third Parties
FHIR simplifies connections with:
- Insurance providers
- Health information exchanges (HIEs)
- Digital health applications
- Analytics platforms
This ensures organizations can meet evolving regulatory demands without rebuilding their infrastructure.
5. Faster Regulatory Adaptation
Healthcare regulations will continue to evolve.
FHIR-based systems provide:
- Modular architecture
- API-driven updates
- Scalability for future requirements
This allows organizations to adapt quickly without major system overhauls.
Financial and Strategic Implications
Compliance is not just a regulatory issue—it’s a financial one.
Organizations that delay modernization may face:
- Increased compliance costs
- Penalties and legal exposure
- Loss of competitive positioning
- Inefficient operations
In contrast, adopting a FHIR-based EHR system enables:
- Lower long-term IT costs
- Faster innovation cycles
- Improved patient engagement
- Stronger payer relationships
Taking the Next Step: Transitioning to a Modern EHR
Moving to a FHIR-based EHR system is a strategic initiative that requires planning and execution.
Key steps include:
1. Assess Current Infrastructure
Evaluate your existing EMR/EHR capabilities and identify interoperability gaps.
2. Define Compliance Requirements
Align your roadmap with 2026–2027 regulatory expectations.
3. Select a FHIR-First Platform
Choose a system designed for interoperability—not one retrofitted for it.
4. Implement a Phased Migration Strategy
Transition systems in stages to minimize disruption.
5. Train Teams and Optimize Workflows
Ensure staff are equipped to operate within a modern, API-driven environment.
The Future of EHR Systems Is Interoperable
Healthcare is moving toward a fully connected ecosystem where data flows freely between providers, patients, and payers.
FHIR is not just a technical upgrade—it is the foundation for the next generation of healthcare delivery.
Organizations that act now will:
- Stay compliant
- Reduce operational costs
- Improve care delivery
- Gain a competitive edge
Those that delay risk falling behind in an increasingly digital and regulated healthcare environment.